Territorial medicine has specific characteristics and so do simulations: similarities and differences, plus possible implications for teaching methodology
Introduction
The use of simulation in the medical field originated from an intuition by HD Barrow, an American neurologist and university lecturer at the University of Southern California, in the late 1960s, at a patient’s bedside. During the same period, and still at the same university, the first computer-controlled patient simulator was designed, Sim Uno. In the 1980s D. Gaba guided the design of CASE (Comprehensive Anesthesia Simulation Environment), a complex manikin, placed in a hospital operating room.
These two strands have developed over the years creating different specificities depending on the environment in which they have been used. The initial debate on ‘structured patient’ and ‘simulated patient’ has become more complex: the environment in which simulation is used has become relevant especially in declining the use of methodology and technological tools which are differently subdivided according to the field of action.
In this article we would like to focus on the specificities of the territorial approach, not in opposition to other fields, but by identifying similarities and differences, with implications on the didactic methodology and on the actors and tools involved.

Specificity of the environment of diagnosis and the territorial treatment
Medical sociology, starting from the pioneering writings by Parsons T (1957) and Freidson E (1960), dealt not only with medicine in general, but also and above all with the environment in which it was practiced and how this changed the very clinical management of patients. Freidson argued that when local patients go to the doctor very often they come ‘prepared’ with an idea of diagnosis and therapy already formulated in their head. Local patients are in control of which of the doctor’s (or health care provider’s or educator’s) directions to follow, whether or not to do investigations, whether or not to go to specialists, whether or not to stick to treatment. They also consult with friends, relatives, people they consider to be health literate, in addition to the ubiquitous Dr. Internet.
This implies not much of a difference in values of humanitarian approach, but a precise difference in field of action and method, including in training. (McWhinney IR, 1993; Salvestroni F, 1968)
For example, the distinction between hard and soft skills, whether it is useful like the teaching basis, seems not enough for territorial simulation practice, when it comes to certain educational needs that allow the healthcare professional to ensure the safety, taking charge and process of diagnosis and treatment of the patient.
Simulation and territory.
Although our experience with simulations also covers educational courses for various health professionals, e.g. nurses, medical students, and other health workers, in these reflections the focus is on general medicine doctors for whom we have conducted lots of simulations over the past 15 years.
Some characteristics of territorial simulations
First of all, it must be considered that the territory is an environment for which a holistic approach is necessary. Without going into detail on the concept of ‘holism’, we intend that teaching for those who work or are about to work in the territory must be done by focusing on clinical, management and relational aspects at the same time, concentrating, depending on the context and the classroom, on the aspects that emerge as priorities or critics.
In the first simulations, especially for those who are unfamiliar with simulations, the three aspects must be dealt with attention, especially the relational one, which must be inserted gradually. In the territory, in fact, patients are likely to bring into the consultation the values, beliefs and ‘common sense’ of the community in which they live. Very often, professionals and territorial health workers are also part of the same community.
The concept of fidelity in territorial simulations
The traditionally low use of technology in the territory allows us to focus on two critical aspects which are the logical (clinical) pathway of the practitioner and the intersubjective management of health and illness experiences.
In education, since the very beginning of the simulation practice, we have raised the issue of realism or ‘adherence to reality’. Very often participants complain that “if I had had a real patient in front of me” it would have been different. This statement often prompted us to present the simulation to the learners as “a bridge between theoretical and practical learning”, emphasizing the similarity with climbing gyms for those learning to climb and the dimension of reality. It is clear that as ‘faithful’ as simulation is, the practice in the field, guided by a tutor, is different.
The concept of fidelity is very important in error detection and avoidance practices, especially in particular critical situations where patient safety may be at serious risk.
The term simulation fidelity is traditionally used to define the degree to which a simulator replicates reality. Although there is no unanimous consensus in the literature, we can define fidelity into three dimensions:
1 – materials/equipment fidelity, concerns the degree to which the simulator and equipment duplicate the appearances and sensations of the real world.
2 – environment fidelity, concerns the degree to which the simulator and the simulator environment reproduce motion, visual, auditory, that is generally sensory-type experiences.
3 – psychological fidelity, depends on how well the learner perceives that the simulation is a credible surrogate for that particular training. In other words, psychological fidelity includes all the aspects that determine whether those being trained will perceive that their performance in the simulator will be replicated in real life.

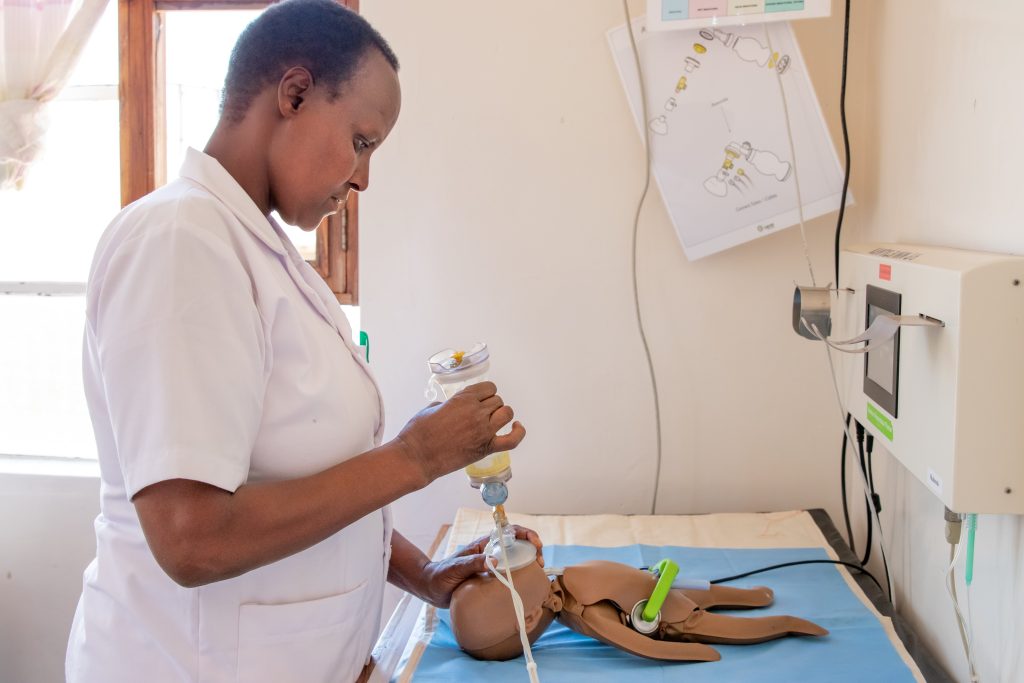
Achieving a high level of fidelity is perhaps easier in those critical situations, such as those that often arise in the emergency department, in which the equipment and environment fidelity is reproducible and is able to be recreated. Otherwise, in a home situation, where several health care providers intervene for a psychiatric crisis, for example, but also for a medical emergency, in the presence perhaps of law enforcement and other actors, it is much more difficult to recreate a high-fidelity environment. What is critical in the territorial setting is the interaction between the different intervening figures: neighbors, onlookers, even the parish priest in some settings, who interact with the patient. This makes the work environment often unpredictable and turbulent.
Therefore, we thought of including another indicator that should be balanced with others, and which is more easily articulated than “psychological fidelity” but can be integrated with it. The concept is what we call “relational intensity.” This is different from psychological fidelity which means that it only describes an interaction between humans, or groups of humans. For example, during a hospital in situ simulation, in the emergency room, the presence of family members may involve medium or high relational intensity, regardless of the use of highly faithful technologies. Relational intensity takes into consideration both the interaction with the patient, but also the subjective experiences of the health care provider and the need for some awareness of these. Extending Schon’s concept of reflection during action, we could say that it considers the level of emotional and affective awareness during action. Relational intensity depends, therefore, on the context in which the process of diagnosis and treatment takes place and is very much related, in the educational setting, to the characteristics of the learner. It can be treated in different ways, but it is always useful, if not necessary, to define the presence and degree.
Soft skills in the territorial simulation
Another concept to dwell on is that of soft skills (or non-technical skills) which usually refers to psychological (and also social) and relational components. However, if we accept the complexity of the mind, as proposed by neuroscience in the last twenty years, even with different viewpoints still under discussion, soft-skills appear complex to teach and assess. It is even more complex in the field of territorial medicine, where relationship management is embodied in the clinical and management of the care process itself.
Moreover, complex territorial simulations require an approach that takes into account not only clinical reasoning but also at least partially the practitioner’s experiences that interfere, for better or worse, with clinical and management. This is more relevant in complex territorial situations (terminally ill, Nursing Home, etc.).
In the territory, simulations can be done with simple devices. Very often, it is much more useful and functional instead to have a “live simulator,” or a well-trained actor.
It therefore becomes necessary, along with the training of simulation facilitators (with different types of skills related to the type and context of simulation) to design the training and “maintenance” of a group of simulators or actors.
Conclusion
The very rapid expansion of the use of simulation methodology around the world has also broadened the areas of implementation and given rise to the need for methodological “specialization” depending on the context. Indeed, there are contextual specificities that make it necessary to differentiate the method according to the environment of use.
It opens a new era for the simulation world to our view, where there are common paths both in method and in the training of those working there.
Finally, it becomes imperative that new professionals, who now work without a role and recognition, such as simulators/actors, be institutionally recognized and properly trained.
| BIBLIOGRAPHY Parson T (1957). Sociologia della Medicina, Feltrinelli, Milano 1977. Freidson E. Client control and medical practice. (1960) Trad. it: Il controllo del cliente e la pratica professionale del medico, in: Maccaccaro A ed altr (a cura di) Sociologia della medicina Feltrinelli Milano 1977 McWhinney I.R. Why we need a new clinical method. Center for Studies in Family Medicine, Dep. of Family Medicine, The University of Western Ontario, London, Ontario, Canada, Scand J Prim Health Care 1993: I I: 3-7 Salvestroni F., “Il medico della persona” Vallecchi Firenze 1968 D. Nestel, M. Bearman. Simulated Patient Methodology – Theory, Evidence and Practice -, published 2015 John Wiley & Sons Ltd, The Atrium, Southern Gate, Chichester, West Sussex, PO198SQ, UK |
READ ALSO