In his book “The dolls’ engineer”, Willem van Meurs tells us about his experience over the last 3 decades in healthcare simulation research and industry. And he points out the impact that medical simulation has had on education and clinical performance.
Willem van Meurs, in his autobiography “The dolls’ engineer” introduces to us his personal experience over the last 3 decades designing patient simulators for healthcare education and training. Already during his early career Willem wore multiple hats, including researcher, educator and technical translator. In 1992, he was invited by professor Jan Beneken to participate in the Gainesville Anesthesia Simulator project together with other clinicians and engineers of the Department of Anesthesiology of the University of Florida. From then on Willem devoted himself to the field of medical simulation. In this short book we’ll follow him from childhood to the present day.

With this book we launch the SIMZINE Library, our new publishing venture, in which we will talk about the people, simulators, and technologies that have had the greatest impact in the field of clinical simulation. Willem’s autobiography is the first in the SIMPEOPLE series, dedicated to the life stories of leaders in the world of healthcare simulation.
- Hello Willem, thanks for your time to be here with us. Firstly, can you tell us what made you decide to write your autobiography?
While waiting for co-authors of two other books I had in the pipeline, I had started to write down my somewhat convoluted personal and professional journey for my children. Then I met an old friend who was writing her own autobiography, and she encouraged me to continue and possibly take it a bit more seriously. This encouraged me to send a sample chapter to SIMZINE Editor-in-Chief Pier Luigi Ingrassia, who came back with an enthusiastic response. Due to the change of target audience, we jointly and carefully nudged the content in the direction of my three decades in medical simulation.
- Can you explain how you have contributed to the development of simulation in medicine? What projects or research did you lead or participate in?
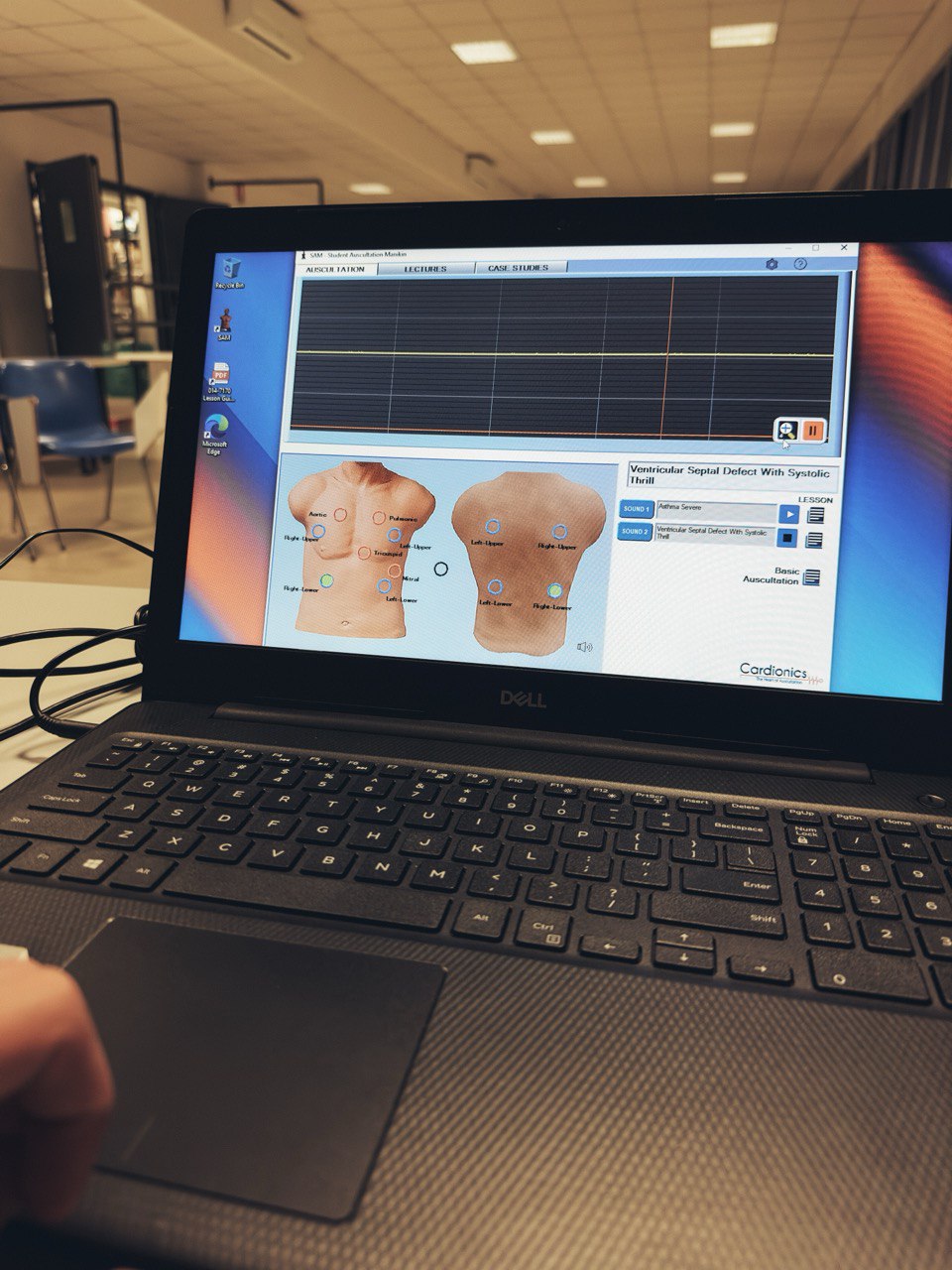
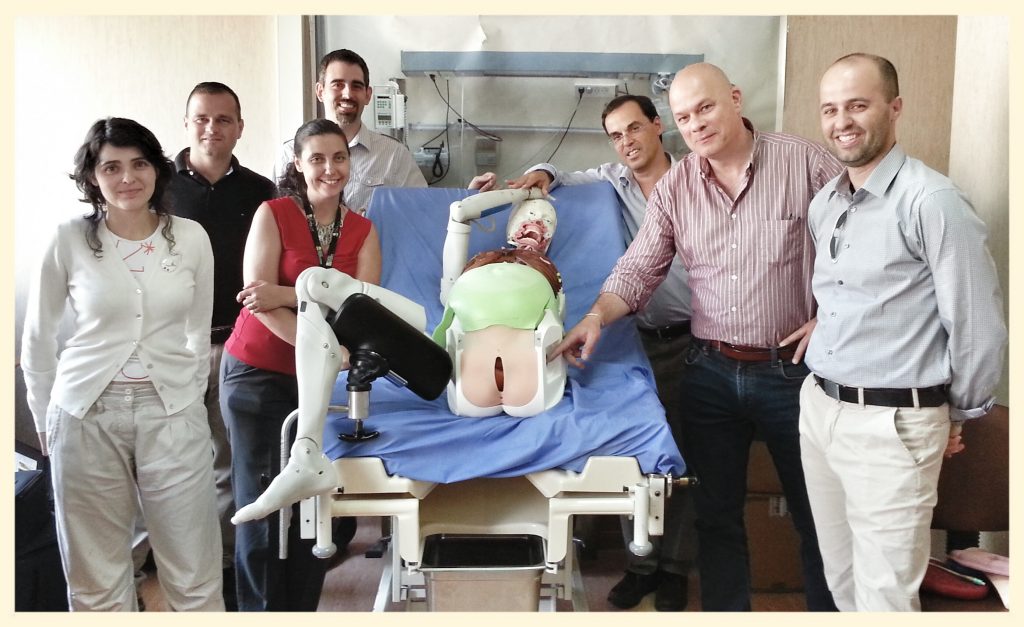
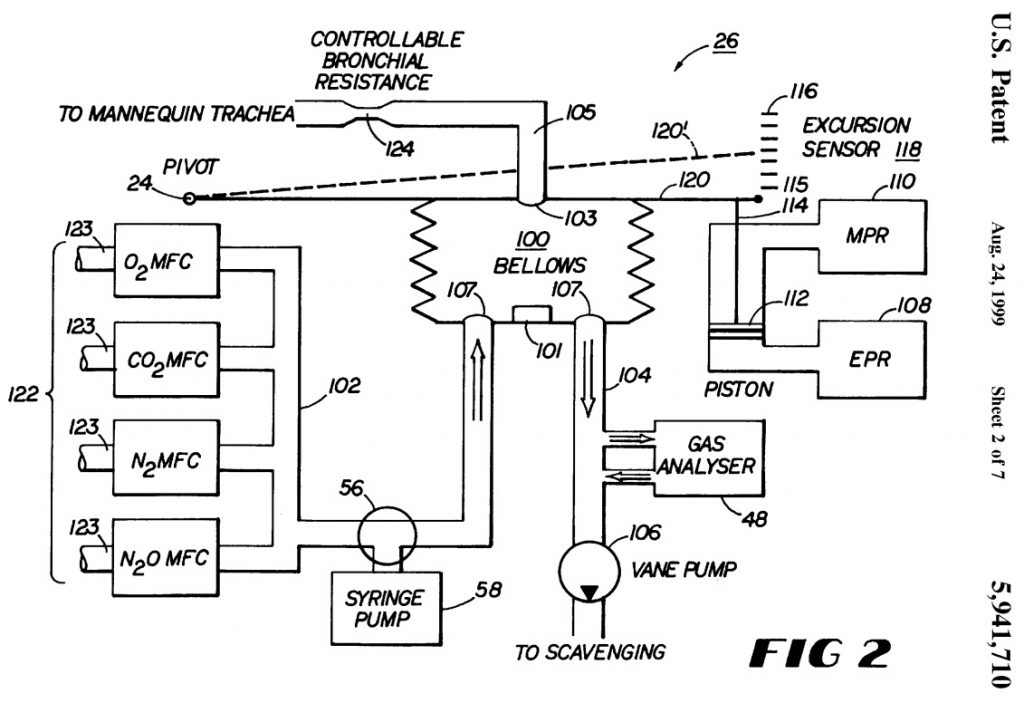
My initial involvement concerned the development of mechanical and mathematical models of physiology and pharmacology of the Human Patient Simulator (HPS), developed at the University of Florida, and commercialized by Medical Education Technologies, Inc., now CAE Healthcare. I led a small modeling team, part of the encompassing HPS team led by anesthesiologist Dr. Michael Good. At the turn of the century, together with obstetrician Dr. Diogo Ayres de Campus, we set up a team of investigators that developed the Lucina childbirth simulator at the University of Porto. I created and taught several classes in modeling and simulation, and in 2011 I published a book on the subject. To assist acute care physicians, thinking about complex and fragile patients under time pressure, neonatologist Dr. Timothy Antonius and I developed the concept of explanatory models, and published that in 2018. During most of this time I was actively involved with the Society for Simulation in Europe (SESAM), which I presided from 2005 until 2007.
- How do you see the impact of medical simulation on medical education and clinical performance?
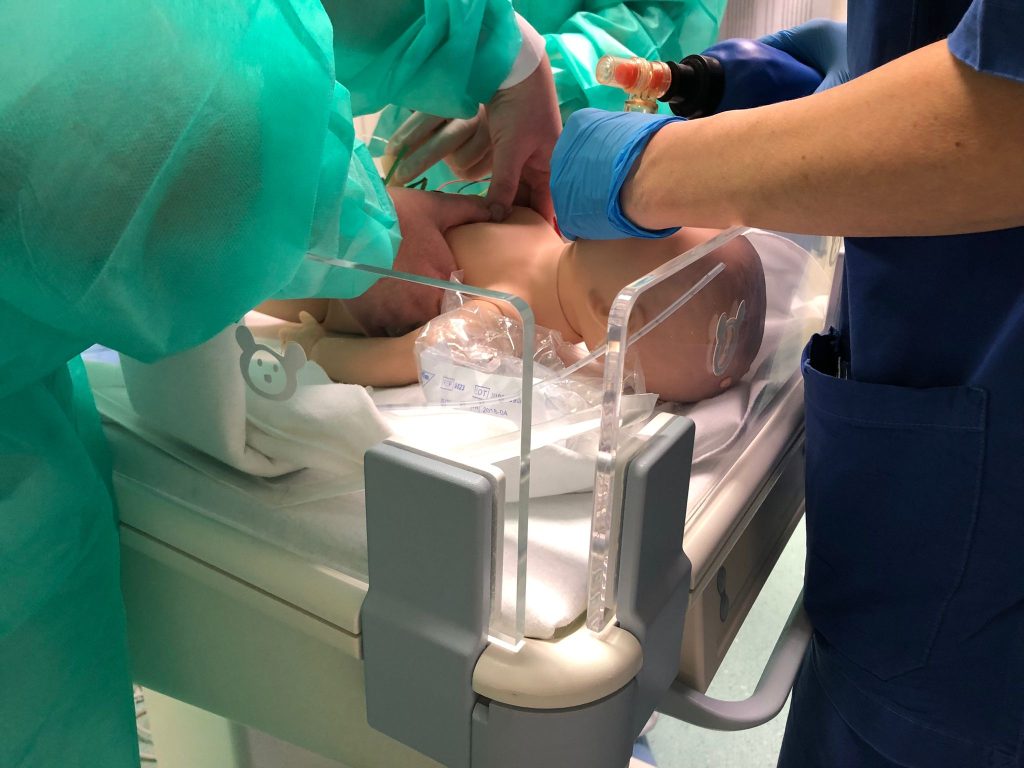
Training on passive dummies, animals, and real patients have been all but replaced by medical simulation based education (MSBE). MSBE has the additional advantage that the training content can be presented at will. Trainees no longer have to wait before incidents occur spontaneously, and are allowed to intervene in simulated critical events. The same clinical performance can now be achieved in less training time, or better performance in the same time.
- What innovations or changes in medical simulation excited you mostly?
The use of mechanical and mathematical models of human physiology to make a machine breathe, die, and be resuscitated like a human being.
- Can you share an example of how simulation had a significant impact on a specific clinical case?
My colleague at the University of Twente, simulator instructor Dr. Benno Lansdorp taught one of his students cardiopulmonary resuscitation (CPR) on an HPS. A week or so later, he suffered an unexplained cardiac arrest himself. His life was saved by the same student who, until then, had never done CPR on a real patient.
- Where do you see the future of simulation in medicine and what role do you think it will play in future medicine?
I expect that explanatory models will allow for a more intuitive, predominantly visual, understanding of underlying physiology, and thereby lead to safer, more effective communication and interventions. “Medical digital twins”, developed in the simulation context, could become run along platforms in the clinic, providing early warning of deterioration of patients, and on which therapeutic interventions can be tried out first, before applying them to the real patient.
- Is there anything you would have done differently looking back on your career?
To be more tolerant of my own and other people’s limitations.
Thank you so much for taking time to share with us your own story. We are convinced that our readers will get inspired by your story, which spans 30 years of evolution in medical simulation. Again, we highly appreciate what you have contributed to this field and we are looking forward to your new research achievements in the future.
READ ALSO