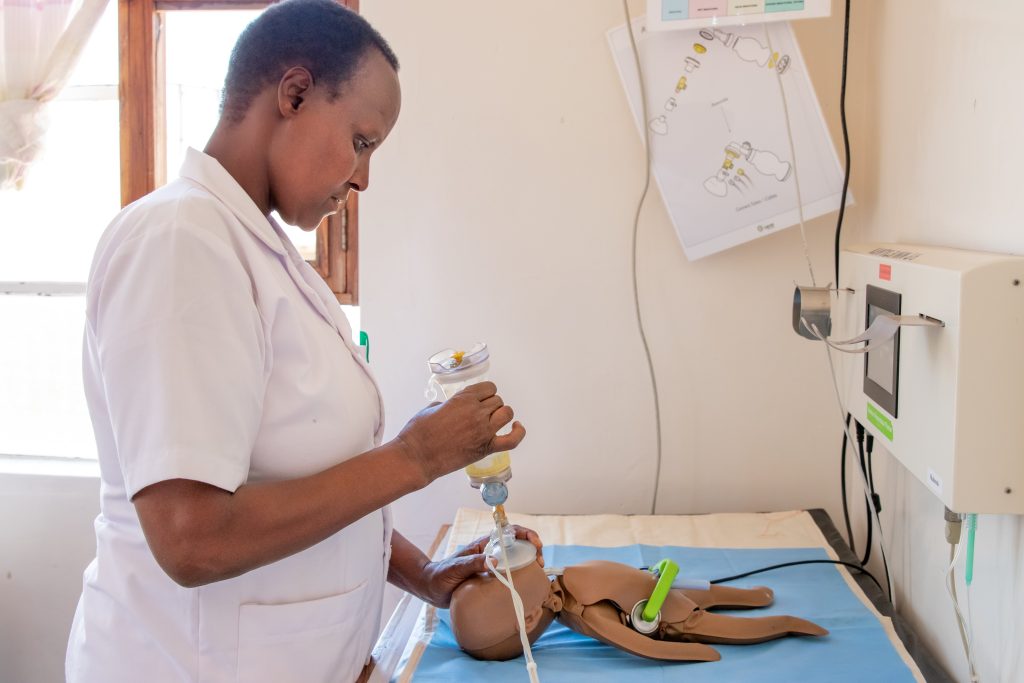
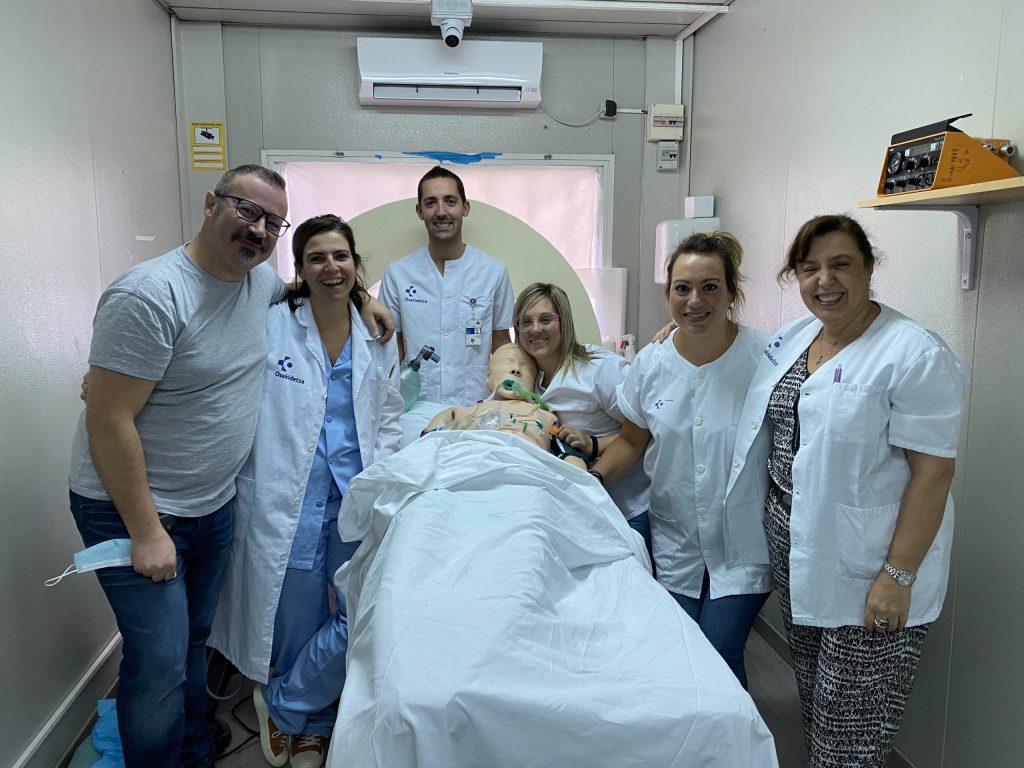
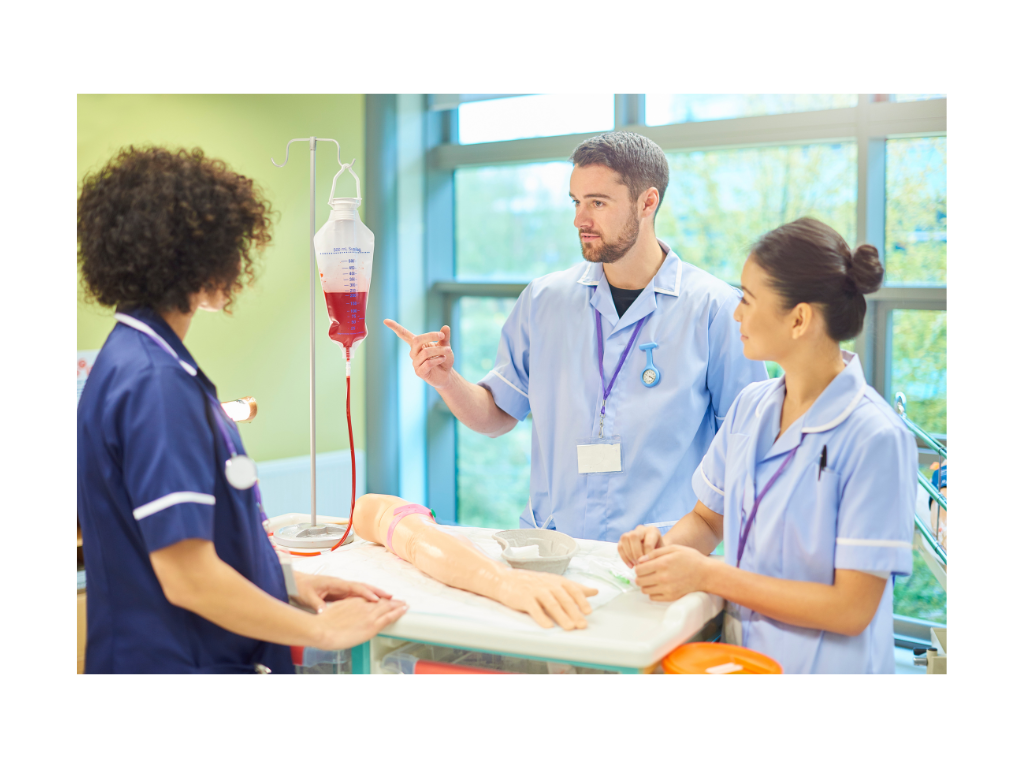
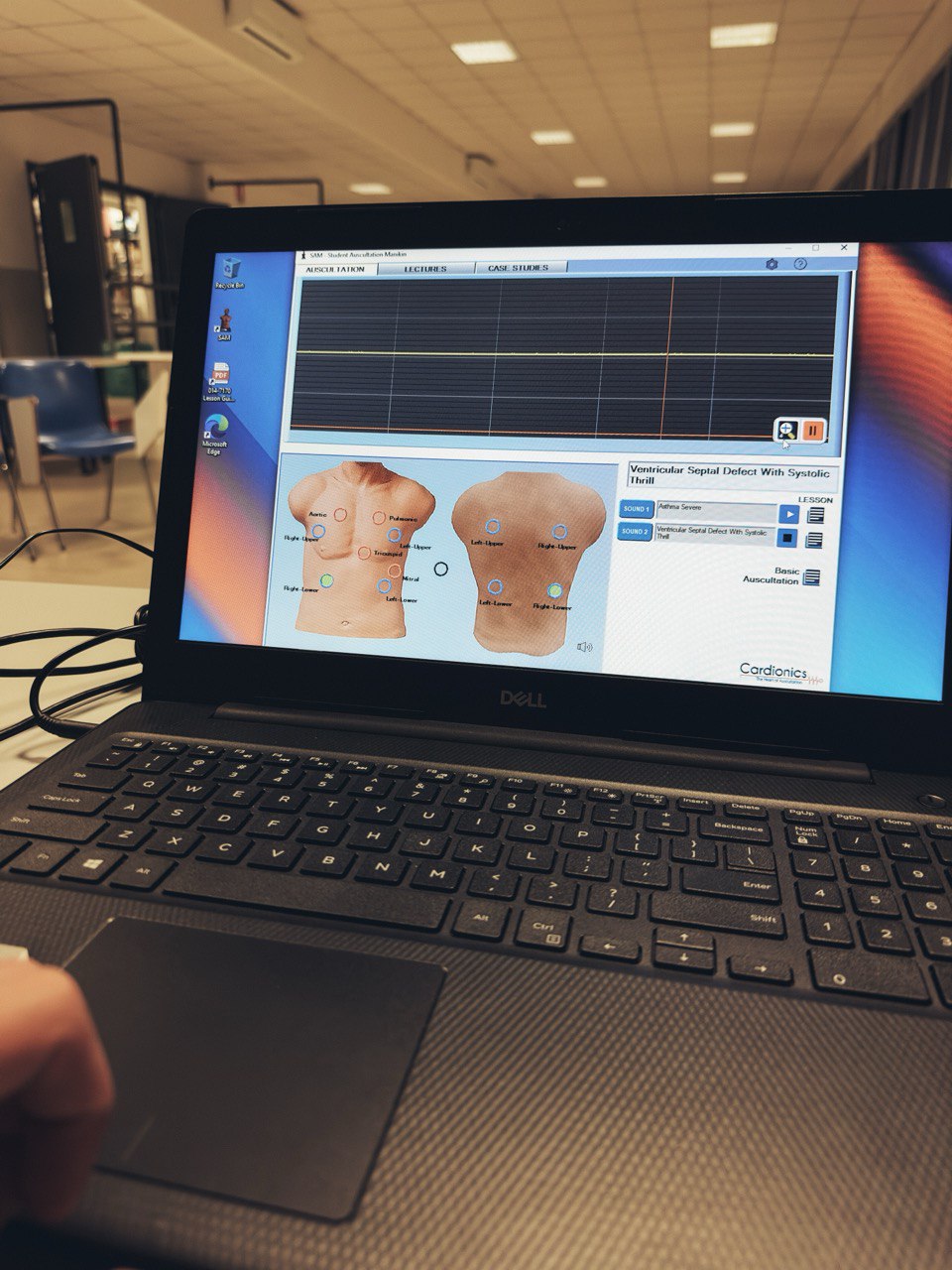
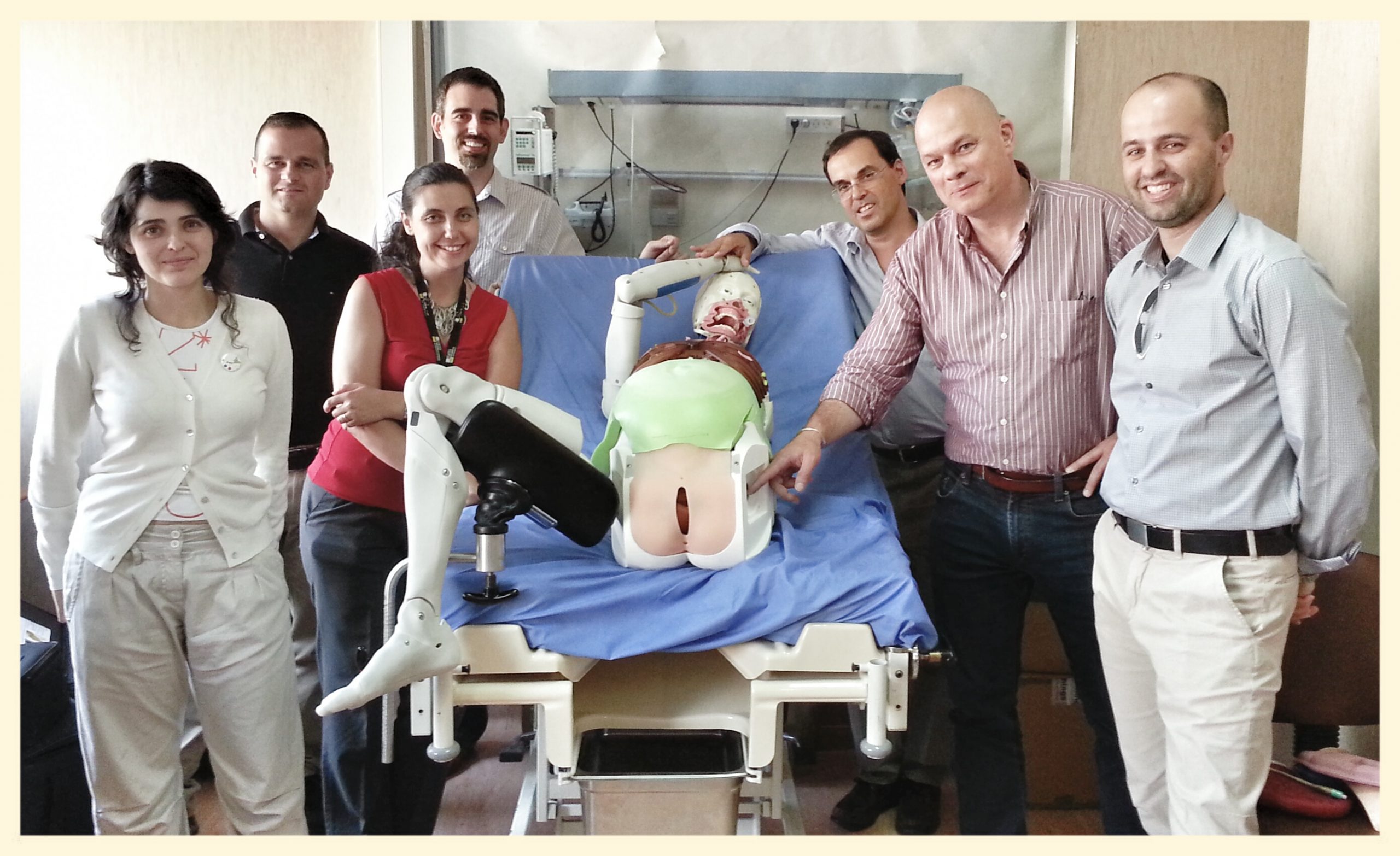
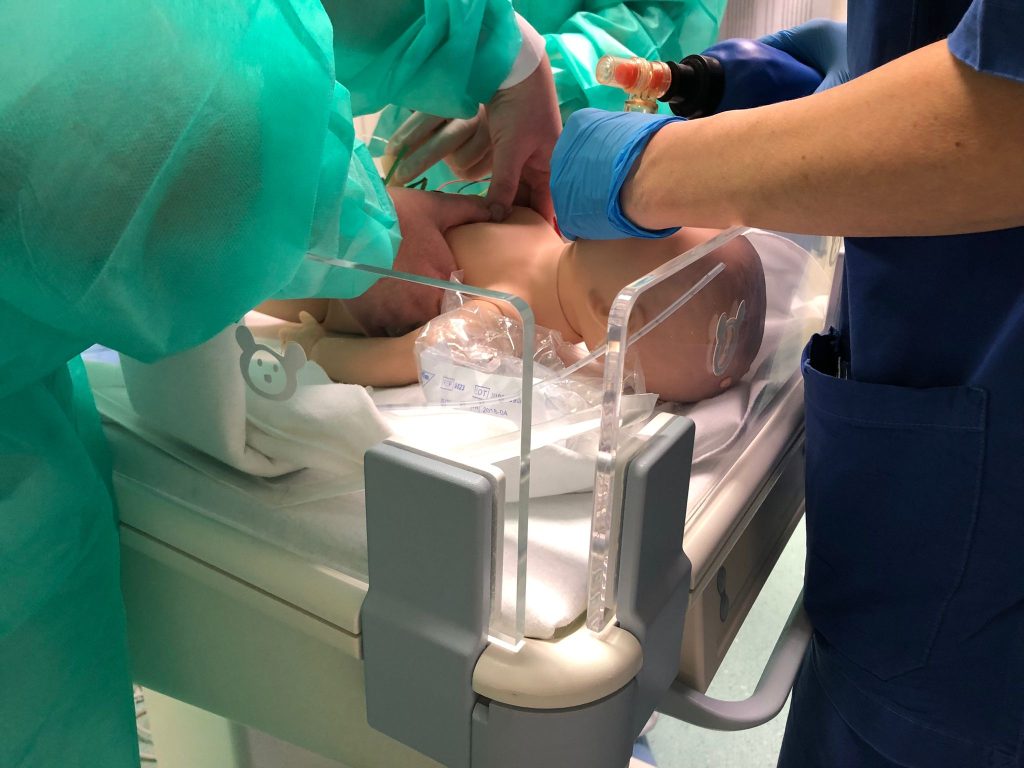
So far simulation has been used almost exclusively for clinical training. Its advantages are increasingly evident both for trainers and for those who participate in simulation experiences. Simulation creates, in fact, that incredible -and perhaps unique!- opportunity for which it is possible to learn by utilizing the error as a resource, without consequences for the patient. However, as the cost of implementing quality simulation is often much higher than traditional teaching and training methods, the value it provides to an organization or system is hard to be immediately understood and appreciated by our executive leaders. Too often when we promote simulation we associate it with training courses, university or continuing education, and we demonstrate its effectiveness in terms of participant satisfaction and the ability to develop procedural and relational skills. In fact, the value of simulation goes far beyond just being a training tool. The scientific literature indeed has amply highlighted how training based on simulation and experienced in appropriate places (simulation centers) or in real healthcare environments (in situ), guarantees many potential benefits for patient safety, ranging from error prevention to damage control. It represents an essential tool for improving the level of reliability of the operators and, more generally, of the system within which the workers operate, taking into account the complexity of all the elements with which they must interface. We are therefore talking about “human factors”, that is the domain of disciplines ranging from psychologyto ergonomics, from architecture to engineering, which seeks to improve safety and efficiency by using the “human component” of the system to its maximum performance. By applying the principles of planning and design, and by simulating scenarios and behaviors, the physical environment where the man -and hence the health professional- works can be modified, the decision-making process can be improved and organizational efficiency and safety can be increased. At each level, different types of simulation, chosen with competent professionalism and appropriate experience, can help test potential weaknesses or identify actions that are most likely to cause errors. A modus operandi that uses a sequential process of testing, tweaking and retesting can only bring incremental improvements, making it easier for us professionals to do the “right thing”.
Recently the Ministry of Health has set up a technical working group to promote simulation in health care. I can’t help but share not only with health professionals, but with the whole of our community (composed of potential patients!) the satisfaction that it was the Ministry of Health, and not that of University and Research, that took this important step. Simulation must become an integral part of the health system of our territory. Certainly starting from the training of its operators, but not limited to this.
It is good to stop referring to simulation only in association with training, the decanted simulation courses. We -health education professionals first- should all start to talk about patient health (also) through simulation.
READ ALSO