Álvaro Trampal Ramos, aka @enfermerodesimulacion, tells us about the 5 main myths about clinical simulation that nursing students face.
Year after year, course after course, scenario after scenario, the simulationists are learning, improving and making changes to the scenarios with the aim of offering the best learning experience to our students through clinical simulation.
On many occasions, we fall for myths or actions that we consider to be correct, but as we experiment, study and learn, we realize that they are wrong.
In this article I am going to talk about 5 myths that we can fall into when we delve into simulation with nursing students and, in general, in any simulation scenario that we carry out.
#MYTH 1. INVESTING IN HIGH-TECH SIMULATORS GUARANTEES SUCCESS.
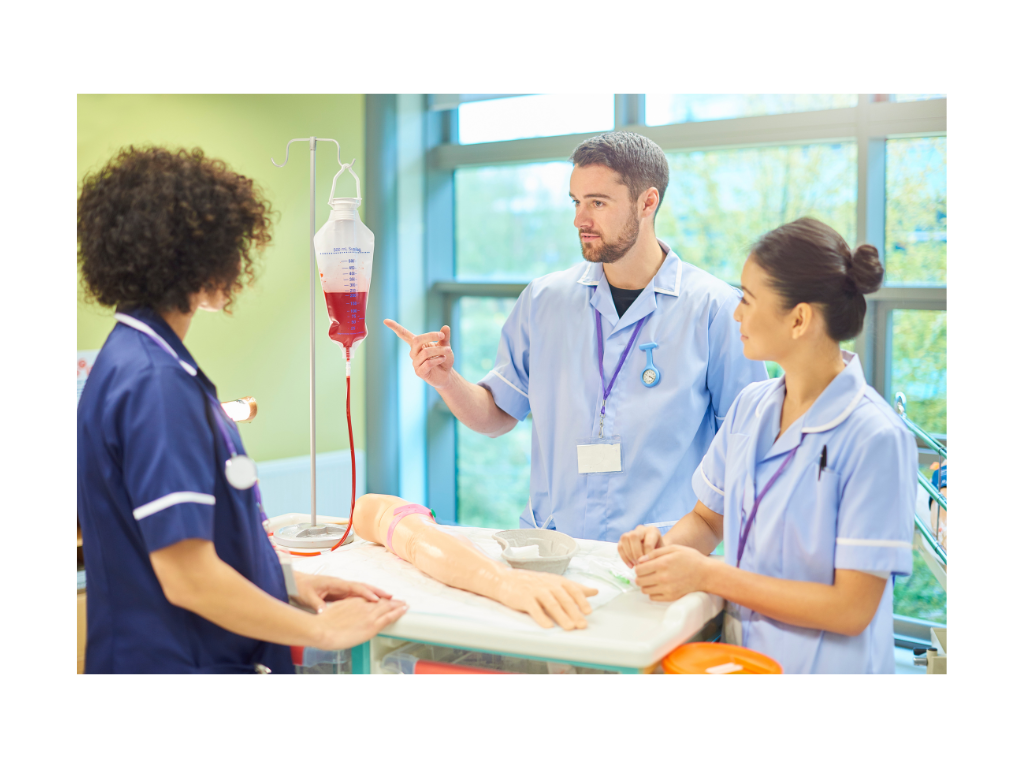
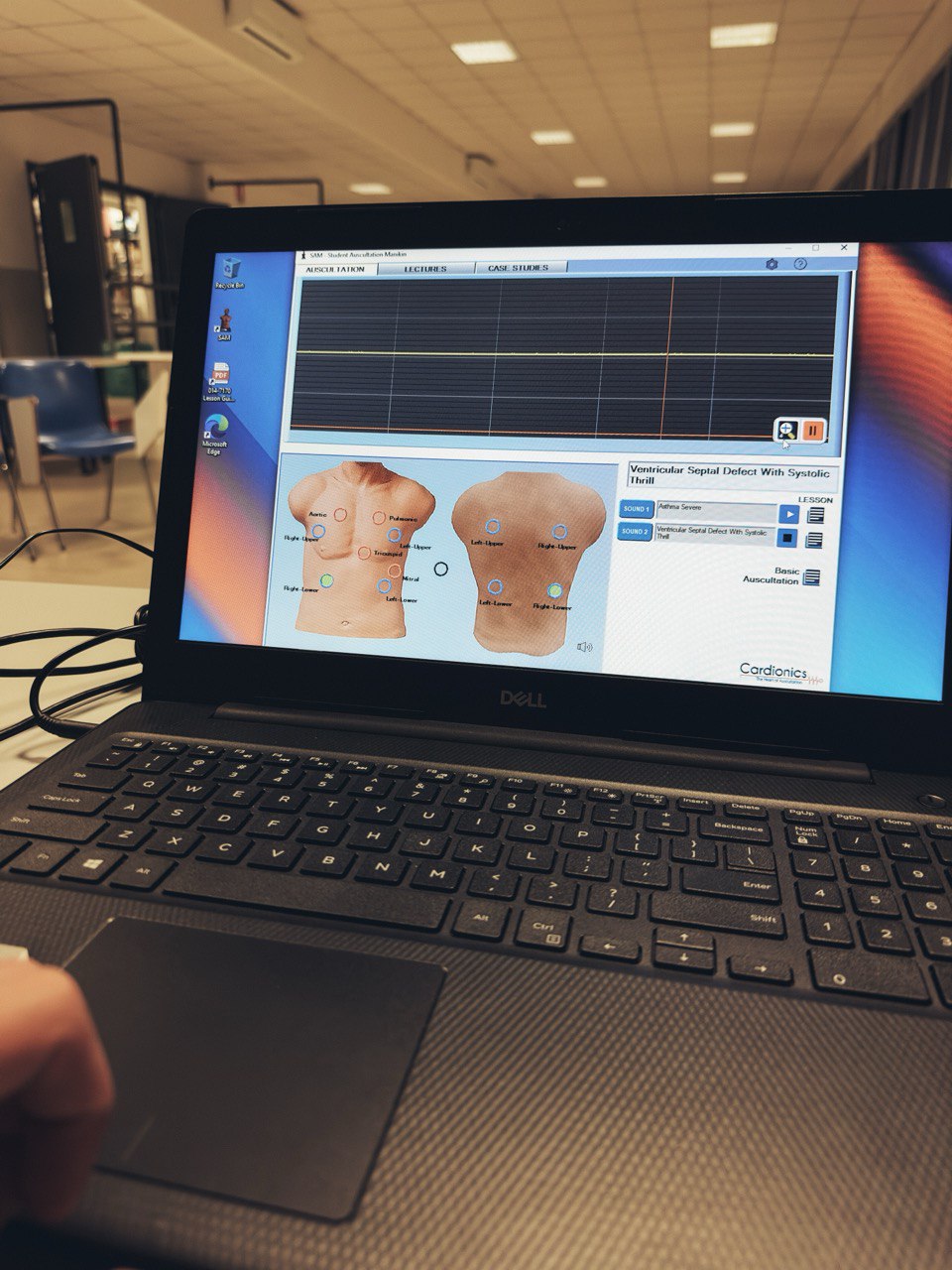
I never get tired of repeating it, the most expensive and most technological tools are not always the best for the simulation that we have designed. We will have to previously analyze the needs of the scenario, the learning objectives and the expected competencies of the students. A scenario for first-year nursing students whose objective is the management of a patient with orthostatic hypotension, in which we will not require a high-technology simulator as we can even use an actor, is not the same as a scenario for fourth- or postgraduate students, in which we will train an advanced life support scenario that requires an anamnesis by the students, administering medication, intubation, defibrillation, and so on.
# MYTH 2. THE MORE COMPLEX THE SCENARIO, THE BETTER.
The scenario design is fundamental: we must be very clear about our objectives, as well as the skills of our students. Remember that the scenarios are designed for students to learn through critical thinking, not for the instructor to show off everything he knows. A first-year student will not be able to carry out a zone 3 scenario on Acute Pulmonary Edema when they have not yet taken the subject of Medical Pathology or Medical-Surgical. We will adapt the scenarios and, therefore, the objectives to the knowledge that they have previously acquired in the classroom (zone 0) and in the skills workshops (zone 1)
#MYTH 3. THE SIMULATION PROGRAM IS INDEPENDENT FROM THE REST OF THE UNIVERSITY SUBJECTS.
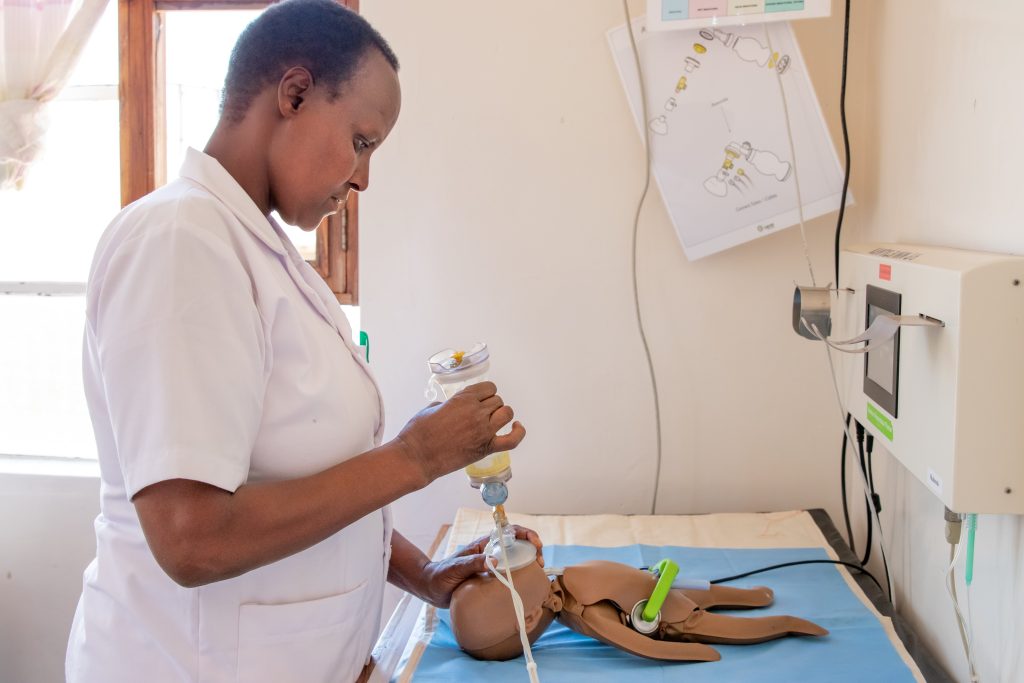
Clinical simulation in health sciences is an excellent tool to give context to the knowledge acquired in the classroom. Students can apply and understand what they have learned through a clinical context and thus be able to acquire the necessary skills to apply the best care to their patients in their clinical care activity. That the student can carry out techniques or scenarios on a manikin/actor, before living it in a real situation, is an excellent opportunity to learn, improve and increase clinical safety.
#MYTH 4. IT IS NOT NECESSARY TO INVEST IN AUDIO OR VIDEO IN THE SIMULATION LABORATORY.
We can say that the video, and especially the audio, is the main element of torture for all of us who perform clinical simulation. Little by little, the industry and the companies that are dedicated to the design of simulation laboratories are managing to optimize the audio in the rooms and the angles of the cameras, making the simulation experience clearer, in such a way that both facilitators and students who are watching the simulation scenario do not miss important details. In my humble opinion, having had many headaches with audio and video systems, I believe that good planning and counting on experts are important to ensure the best possible audio and video.
# MYTH 5. YOU DO NOT HAVE TO PREPARE THE SIMULATION, OR DESIGN IT.
Whenever I can I say it: clinical simulation is not a game. It is necessary to design the simulation scenarios previously, having the objectives of the scenario, fidelity, timeline, necessary material, decision algorithm and a long etcetera, that is, all the necessary elements for the clinical simulation scenarios to be successful and for us to achieve the objectives marked. It must be remembered that it is essential to carry out the piloting of the scenario, that is, to test it beforehand to realize possible design errors.
In these five myths I wanted to reflect the beliefs that we may have when we start with clinical simulation and especially with undergraduate nursing students. There are many other myths or beliefs such as the importance of simulation technicians, debriefing, the need for a “psychological safe container” and a long etcetera that arise once we delve into simulation, but we will leave these for another time. I hope you liked this little article.
Would you like to know more? Find out more in the Instagram video by @enfermerodesimulacion (Spanish language):

READ ALSO