How simulation played a key role during an emergency in an emergency: the story and experience of an ICU nurse.
My name is Daniele. I am a nurse from Calabria with 16 years of service in intensive care, ICU CCH at the Materdomini University Hospital of Catanzaro.
I wanted to share my work and simulation experience during the SARS-CoV-2 pandemic in the structure where I work.
We were at the end of 2020, Calabria had been slightly hit in terms of cases and deaths during the first wave. However, as the monthly positive trend showed no signs of abating, health agencies, including mine, began hiring various health professionals, including new nurses, to deal with the pandemic.
Heroes! This is how the media called healthcare workers for months. Some with great experience, many others with little or none, the operators were assigned to infectious disease wards and especially to intensive care, where the level of assistance is extremely high and requires knowledge and skills on the part of the nurses that cannot be acquired in a short time.

The circumstances, as you can well imagine, were not the best. I saw and lived hour after hour extreme situations and emotions: anger, tension, fear. Desperation and lack of organization were often dominating.
That is why I was contacted by my area managers, principal, deputy and coordinator, who gave me the task of coordinating and training the new recruits, with the aim of being able to better face the new wave that was about to come.
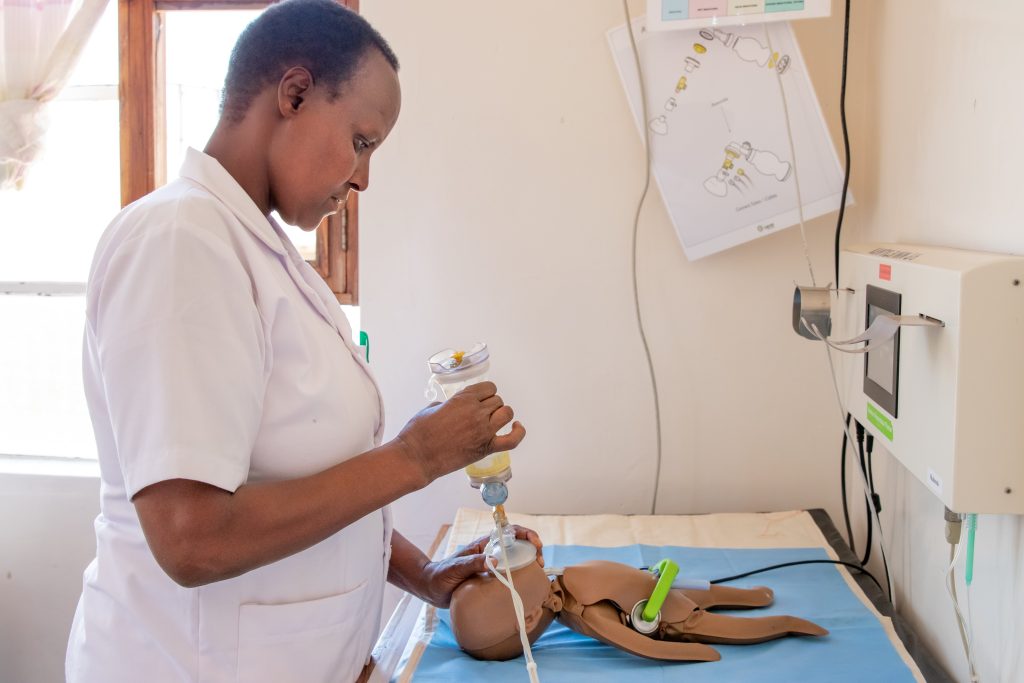
The time and data of the pandemic were not on our side. The training process had to be as fast as possible. This was how, during the first few shifts in the COVID19 area, I thought I could meet the many needs of the nursing and healthcare workers’ group by organizing short simulation training sessions in a dedicated room outside the COVID19 unit.
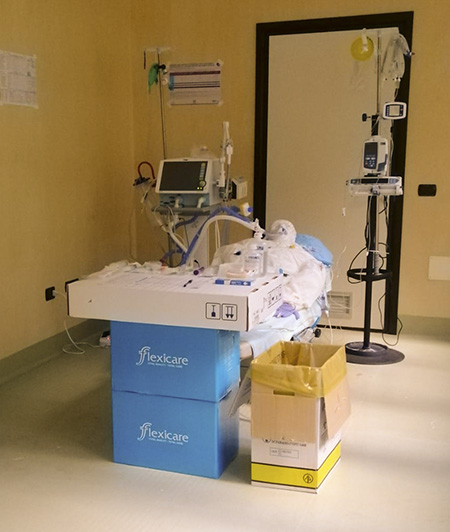
This room was created and assembled in a few days in the free moments after the shift: it reproduced in a very realistic and faithful way the ICU station / box with relative columns, electromedical devices, aids, medications used and obviously the hospitalized patient.
The hardest part of those extra shifts was finding a manikin that could simulate the various situations, everything was stopped by the lockdown! And so I looked around and saw something that had the silhouette of an adult person: the defective overalls that accumulated from shift to shift. I took one, started filling it with cushions of various sizes to give it thickness, placed it on a disused ambulatory bed found in a warehouse, filled some shoes to make the left and right feet, and filled disposable gloves with water to create the hands. Everything was taking shape. The fatigue of the extra shifts was beginning to be felt, but the desire to be able to lend a hand to the colleagues who had just arrived gave me the strength to continue and dare more.

Only the head was missing, the most important part. I remembered having a white mask used in the carnival at home. I added holes near the nose and mouth. I dared even more: with a test lung connected to a mechanical turbine ventilator, through an endotracheal tube passed through the hole made in the mouth and placed in the chest, we simulated the lungs and the consequent expansion of the chest. With another balloon, placed lower in the abdomen, I simulated the stomach with its gastric nasal tube passing through the hole made in the nostrils. I then connected a bladder catheter to a classic infusion set with a 1000 physiological bag to simulate diuresis. Still not satisfied, I added the various devices such as a cvc trilumen in the left jugular, a dialysis bilume hermetically connected to a 1000 SF bag with 5 cc of iron to simulate venous blood in the left femoral area, an arterial cannula for invasive monitoring of pressure connected to the respective kit, and 2 peripheral venous accesses. I finally moved on to basic monitoring: I borrowed the cables normally used for ECG, SpO2, Tc, invasive P.Art and connected everything to the station/PC with its monitor. Then I started the “Waveform and Parameters Simulator” test software. Luckily I had read the updated manual some time before 😅.
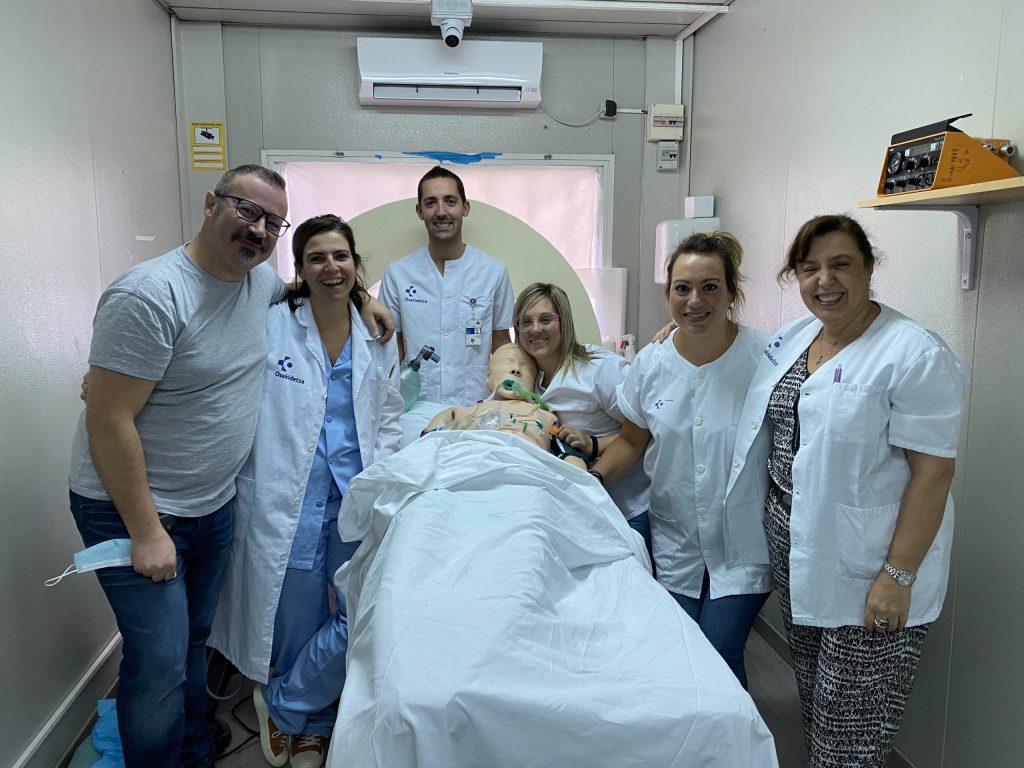
Before the different sessions, almost as an instinct, I preferred to speak personally with all of them, encouraging and motivating them, involving both the health workers and the doctor in order to understand, from their point of view and with their words, what was okay and what wasn’t during the first few rounds.. We started by handling several basic routine situations, from venous access to cardiac arrest and the application of ACLS protocols.. Although the realism of the simulator was certainly moderate, I observed, with pleasure and satisfaction, that the new colleagues made even more of a team, being able to satisfy their doubts and uncertainties regarding the management of critical patients and, above all, gaining greater self-confidence.
To understand if the simulations had worked and if the objective had been achieved, together with my managers I thought that the only solution was to personally see the colleagues in the different shifts. In a short time I could see that the situation had improved considerably: especially in moments of strong internal criticism, the synergy and collaboration with doctors and nurses had improved significantly.
Now, after so many months of that experience, it occurs to me to rethink the work done and the mental and physical effort required. I would repeat everything from beginning to end: simulation is a tool that cannot be missing in nursing training, guaranteeing greater safety for patients but also for professionals! I hope that universities and health agencies invest more and more in training based on simulation experience, involving the various simulation centers and laboratories.