In this episode of Between 2 Simulators, Susan Gallagher, President of the National Bariatric Solutions Conference, shares her journey as a nurse, ethics expert, and bariatric care advocate. Susan highlights the growing need for specialized care for patients of size, outlining challenges such as IV access, surgical risks, and unconscious bias. She emphasizes the vital role of simulation in training healthcare providers to manage these complexities effectively. Susan also introduces her upcoming conference, which combines hands-on simulation, guest speakers, and vendor showcases to improve bariatric care worldwide.
In a thought-provoking episode of Between 2 Simulators, Susan Gallagher, a prominent nurse leader and President of the National Bariatric Solutions Conference, joined host Jake Rahman to share her insights on the overlooked challenges faced by patients of size in healthcare. With a background in nursing, policy ethics, and bariatric care, Susan has dedicated her career to advocating for improved training, awareness, and equitable care for larger-bodied patients.
From her experiences developing educational programs to her mission of changing perceptions within healthcare, Susan’s insights underscore the urgent need for healthcare providers to embrace more inclusive and compassionate practices — and how simulation can play a vital role in that shift.
A Career Defined by Advocacy and Ethics
Susan’s journey into healthcare was driven by a passion for improving care quality and ensuring ethical treatment for marginalized patient populations. With master’s degrees in nursing and religion and social ethics, and a PhD in policy ethics, Susan’s academic background uniquely positioned her to explore how healthcare resources are distributed — and how patients of size often face systemic inequalities.
“My focus has always been on the just distribution of healthcare goods and services,” Susan explained. “Over time, I became increasingly aware of the unique challenges faced by patients of size — and the lack of specialized training available to address those needs.”
Recognizing this gap, Susan became certified in bariatric nursing and safe patient handling, equipping herself with the expertise to advocate for better care strategies for larger-bodied patients.
The Growing Need for Bariatric Care in Healthcare
During the interview, Susan highlighted the stark reality of rising obesity rates in the United States and beyond.
“Right now, about 42% of the U.S. population is considered obese,” Susan noted. “And in some hospitals, as many as 85% of patients have a BMI greater than 50.”
These numbers highlight the urgent need for healthcare systems to adapt — yet many institutions remain unprepared to provide appropriate care for patients of size. Susan emphasized that this is a global issue, with obesity rates steadily rising across Europe and the UK as well.
Unique Care Challenges for Patients of Size
Susan outlined several key challenges healthcare providers face when caring for patients of size, including:
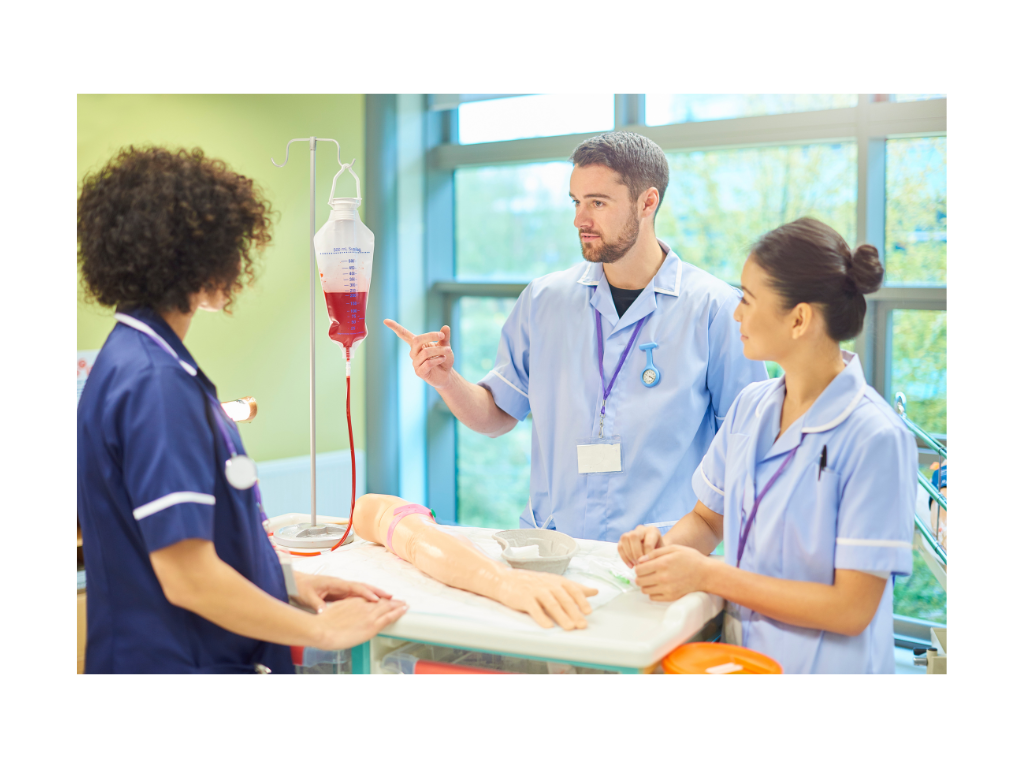
- Difficulties with IV Access — Finding veins in larger-bodied patients can be more complex.
- Intubation Risks — Extra fat tissue can create airway management challenges.
- Surgical Complications — Surgeons must navigate altered anatomy and increased risk factors.
- Skinfold Management — Specialized hygiene care is required to prevent skin irritation and infections.
- Mobility Issues — Moving, turning, or repositioning larger-bodied patients requires specialized techniques and equipment.
Beyond clinical challenges, Susan emphasized the emotional toll these patients experience. Many delay seeking medical care out of embarrassment, fear of judgment, or negative past experiences — arriving at hospitals sicker and in more critical condition as a result.
“Our patients are often afraid to come in because they feel stigmatized,” Susan said. “By the time they do seek care, their health conditions have often worsened.”
Why Healthcare Training Has Fallen Behind
When asked why bariatric care training has been overlooked, Susan pointed to several factors:
- Lack of Awareness — Many healthcare leaders underestimate the prevalence of larger-bodied patients in their facilities.
- Bias and Stigma — Unconscious bias within healthcare systems often leads to judgment and insensitivity toward patients of size.
- Equipment Limitations — Even when facilities invest in bariatric equipment, staff often find that tools intended to support larger-bodied patients don’t function effectively in real scenarios.
“Healthcare providers might think a piece of equipment rated for 1,000 lbs will automatically work for larger patients — but they often overlook width, pinch points, and maneuverability,” Susan explained.
This is where simulation becomes a powerful tool.
The Power of Simulation in Bariatric Care
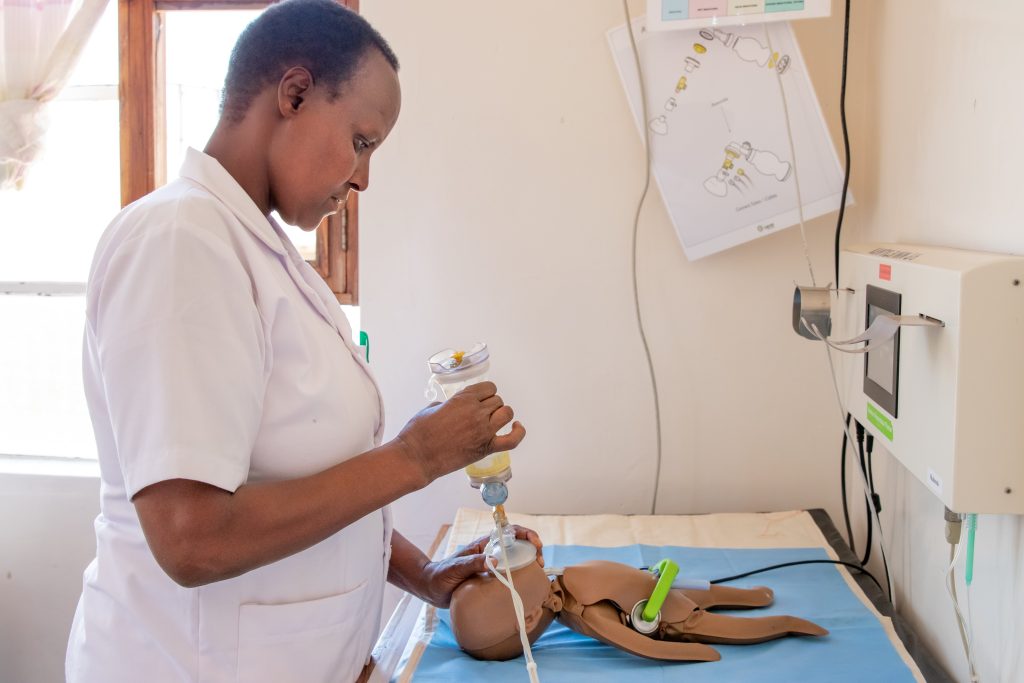
Susan highlighted the vital role that simulation plays in educating healthcare providers on the complexities of caring for patients of size.
“Simulation makes the challenges real for healthcare teams,” Susan said. “When professionals try to lift, move, or care for a larger-bodied mannequin — they see firsthand how difficult it can be and what changes are needed.”
By integrating bariatric mannequins and wearable simulation suits into training, educators can create realistic scenarios that address:
- Safe patient handling techniques.
- Fall recovery strategies for larger-bodied patients.
- Car extractions and emergency response tactics.
- Turning and repositioning practices to reduce pressure injuries.
“These aren’t complex, high-tech scenarios — they’re practical, hands-on situations that directly improve patient care,” Susan emphasized.
Addressing Bias and Building Empathy
One of the most powerful outcomes of simulation, Susan stressed, is its ability to expose unconscious bias and create opportunities for discussion.
“Healthcare teams often giggle or feel uncomfortable when they first encounter a larger-bodied mannequin,” Susan explained. “We can use that moment to have important conversations about empathy, respect, and recognizing our own biases.”
She believes that through structured debriefing, simulation helps foster compassion — ensuring that healthcare providers approach patients of size with dignity and respect.
The National Bariatric Solutions Conference: Driving Change
Susan is also the driving force behind the National Bariatric Solutions Conference, an event dedicated to improving care for patients of size. Now entering its third year, the conference continues to grow in scale and impact.
The 2025 conference will feature:
- 18 hours of hands-on simulation to build practical skills.
- Guest speakers including patients sharing their lived experiences.
- Over 40 vendors showcasing bariatric care solutions.
- Sessions exploring early mobility, skin care, and critical care for patients of size.
“We’re not just talking about obesity policy or metabolic surgery,” Susan said. “We’re exploring every aspect of patient care — from mobility and hygiene to mental well-being and emotional support.”
A Call to Action for Simulation Providers
Susan concluded the interview by emphasizing that the simulation community must do more to ensure that larger-bodied patients are accurately represented in healthcare training.
“Mannequins like the 42 represent a 330-lb patient — but that’s still on the low end for many of the patients we’re seeing,” Susan explained. “We need to expand our tools and scenarios to reflect reality better.”
She encouraged healthcare educators to integrate bariatric-focused scenarios into routine training — ensuring healthcare teams are prepared to care for every patient with confidence and compassion.
“We have a duty as an industry to represent these patients — and to ensure their care is as safe, effective, and dignified as anyone else’s,” Susan concluded.
Conclusion: Leading the Way in Bariatric Care Innovation
Through her advocacy, education, and leadership, Susan Gallagher continues to champion equitable care for patients of size. By promoting simulation-based training, driving awareness through the National Bariatric Solutions Conference, and challenging unconscious bias, Susan is working to build a healthcare system that embraces inclusivity and ensures that every patient — regardless of size — receives the compassionate care they deserve.
READ ALSO